Diabetic peripheral neuropathy is one of the most common — and most feared — complications of diabetes. Up to 50 percent of people with diabetes will develop some form of neuropathy during their lifetime, and for many, it becomes one of the most disruptive and painful aspects of living with the disease.
The burning feet that keep you up at night. The numbness that makes you worry about every step. The tingling that never quite goes away. These are not just inconveniences. Left unaddressed, diabetic neuropathy can lead to serious complications including foot ulcers, infections, and in severe cases, amputation.
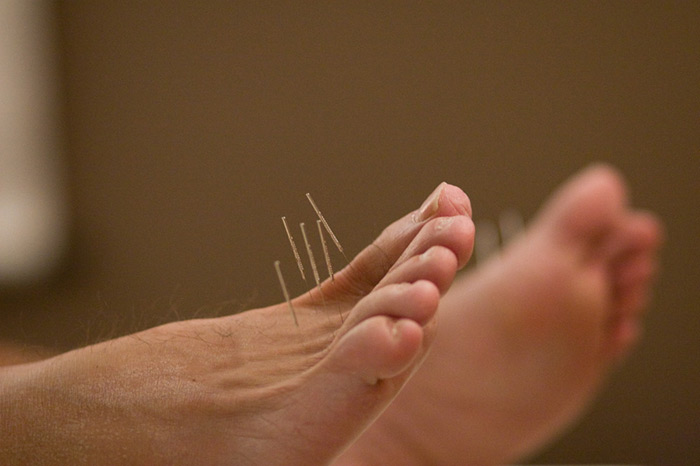
But there is real reason for hope. At our integrative chiropractic and acupuncture practice in Palm Coast, Florida, we work with diabetic neuropathy patients using a comprehensive, multi-modal approach that goes far beyond what most patients have been offered. We combine chiropractic care, acupuncture, laser therapy, shockwave therapy, vitamin B12 injections, and targeted supplementation — all working together to support nerve healing, improve circulation, and reduce pain.
We accept Medicare, making many of these services accessible to our senior diabetic patients. And we take the time to understand your full health picture — because managing diabetic neuropathy well requires more than a prescription.
What Is Diabetic Peripheral Neuropathy?
Diabetic peripheral neuropathy (DPN) is nerve damage caused by chronically elevated blood sugar levels. Over time, high glucose damages the small blood vessels that supply oxygen and nutrients to peripheral nerves — particularly those in the feet and legs, though the hands and arms can also be affected.
The peripheral nervous system includes all the nerves outside the brain and spinal cord. These nerves carry three types of signals:
– Sensory signals: touch, temperature, pain, vibration, and position sense
– Motor signals: commands that control muscle movement
– Autonomic signals: regulation of blood pressure, heart rate, digestion, and circulation
Diabetic neuropathy can affect any or all of these nerve types, which is why its symptoms are so varied — from burning pain to complete numbness to muscle weakness to balance problems. The most common form affects sensory nerves in the feet first, gradually moving upward in a pattern often described as a “stocking and glove” distribution.
What Actually Causes the Nerve Damage?
Understanding the underlying mechanisms of diabetic neuropathy is key to understanding why a multi-modal treatment approach is so effective. Several overlapping processes drive nerve damage in diabetes:
Microvascular Damage
High blood sugar damages the tiny capillaries that supply blood — and therefore oxygen and nutrients — to nerve fibers. Without adequate blood supply, nerves begin to malfunction and eventually degenerate. This is why improving circulation is one of the most important targets in any neuropathy treatment plan.
Oxidative Stress
Excess glucose in the bloodstream generates harmful free radicals that damage nerve cells directly. This oxidative stress overwhelms the body’s natural antioxidant defenses and accelerates nerve degeneration. Several of the supplements we use — particularly alpha-lipoic acid — directly target this mechanism.
Inflammation
Chronic low-grade inflammation is a hallmark of poorly controlled diabetes. Inflammatory compounds damage nerve tissue and sensitize pain receptors, contributing to the burning and hypersensitivity that many DPN patients experience.
Metabolic Dysfunction in Nerve Cells
High glucose disrupts normal cellular metabolism within nerve cells themselves, impairing their ability to generate energy (ATP) and maintain the myelin sheath — the protective coating around nerve fibers that enables fast, accurate signal transmission.
Nutrient Deficiency
Many people with diabetes — particularly those on metformin, one of the most commonly prescribed diabetes medications — develop deficiencies in vitamin B12, a nutrient that is absolutely essential for myelin production and nerve repair. This deficiency can significantly worsen neuropathy and is frequently overlooked in standard diabetes management.
Recognizing the Symptoms — Early and Advanced
One of the most important things to understand about diabetic neuropathy is that early intervention produces significantly better outcomes. Many patients wait until symptoms are severe before seeking treatment — by which point nerve damage can be much harder to address. Here is what to watch for at different stages:
Early Warning Signs:
– Occasional tingling in toes or fingers
– Mild numbness after prolonged sitting
– Slight sensitivity to temperature changes
– Fatigue in the legs after walking
Advanced Warning Signs:
– Constant burning or stabbing pain
– Complete numbness in feet — unable to feel the floor
– Muscle weakness and difficulty walking
– Non-healing wounds or ulcers on the feet
Important: Many people with early diabetic neuropathy have no symptoms at all. Regular foot exams and proactive nerve health evaluation are critical for all people with diabetes — not just those already experiencing pain.
Your Questions About Diabetic Neuropathy, Answered
Can diabetic neuropathy be reversed?
For early-stage diabetic neuropathy, meaningful improvement — and in some cases functional reversal — is possible when blood sugar is well-controlled and targeted therapies are used to support nerve repair. For more advanced neuropathy, the realistic goals are halting progression, reducing pain, improving sensation and balance, and preventing complications like foot ulcers. Earlier action consistently produces better outcomes.
Does controlling blood sugar stop neuropathy from getting worse?
Blood sugar control is foundational — it removes the primary source of ongoing nerve damage. However, blood sugar control alone is often not enough to address the nerve damage that has already occurred, the circulation deficits that have developed, or the nutritional deficiencies that have accumulated. This is why combining good diabetes management with targeted integrative therapies produces the best results.
Is Medicare covered treatment for diabetic neuropathy?
Medicare covers several services relevant to diabetic neuropathy management, including chiropractic care for spinal conditions, acupuncture for chronic low back pain, and certain diagnostic services. At our Palm Coast office, we accept Medicare and will help identify which services are covered under your specific plan. We encourage you to call our office for a coverage conversation before your first appointment.
Why are my feet worse at night?
Neuropathy pain typically worsens at night for several reasons: there are fewer distracting sensory inputs competing with the nerve pain signals, circulation tends to slow during rest, and the weight of bedding on sensitive feet can trigger discomfort. This nocturnal worsening is one of the most disruptive aspects of DPN and a common driver of sleep deprivation and depression in affected patients.
What is the connection between metformin and neuropathy?
Metformin, one of the most commonly prescribed medications for type 2 diabetes, is known to reduce the absorption of vitamin B12 from the gut — sometimes significantly. Since B12 is essential for myelin production and nerve health, long-term metformin use without B12 monitoring or supplementation can worsen peripheral neuropathy. If you are on metformin, ask your prescribing doctor when your B12 level was last checked. We can also address B12 deficiency directly through our acupoint injection therapy program.
How We Treat Diabetic Peripheral Neuropathy
Our treatment approach targets all the major mechanisms of diabetic nerve damage simultaneously — circulation, inflammation, oxidative stress, cellular energy, and nutritional deficiency. No single therapy does all of this. Our program combines:
1. Chiropractic Care — Optimizing the Nervous System from the Spine Outward
Spinal misalignments and disc problems can compound diabetic neuropathy by adding mechanical compression to nerve roots that are already metabolically stressed. Chiropractic adjustments restore proper spinal alignment, reduce nerve root irritation, and improve the overall quality of nervous system function — creating a better foundation for peripheral nerve health. Many of our diabetic neuropathy patients also have concurrent spinal degeneration, and addressing both together produces better outcomes than treating either in isolation.
2. Acupuncture and Electroacupuncture — Evidence-Based Pain Relief and Circulation Support
Acupuncture is one of the most extensively studied non-pharmacological treatments for diabetic neuropathy. Multiple clinical trials and systematic reviews have found that acupuncture reduces neuropathic pain, improves nerve conduction velocity, and enhances microcirculation in affected tissue. Electroacupuncture — which adds gentle electrical stimulation through the needles — provides additional nerve stimulation that supports regeneration.
For patients managing neuropathy alongside concerns about opioid dependence or medication side effects, acupuncture offers meaningful, evidence-supported pain relief without pharmaceutical risk.
3. Cold Laser Therapy and Red Light Therapy (Photobiomodulation)
Photobiomodulation therapy uses specific wavelengths of light to penetrate tissue and stimulate mitochondrial energy production at the cellular level. For diabetic neuropathy patients, this translates to:
– Increased ATP production in oxygen-deprived nerve cells
– Reduced local inflammation and oxidative stress
– Stimulation of nerve fiber regeneration
– Improved microcirculation to ischemic tissue
– Reduced pain hypersensitivity
Laser therapy is applied directly to the feet, ankles, and lower legs — the areas of greatest nerve involvement in most DPN patients. Sessions are painless and non-invasive, typically lasting 10 to 20 minutes.
4. Shockwave Therapy — Rebuilding the Circulation That Nerves Depend On
Shockwave therapy delivers acoustic pressure waves that trigger angiogenesis — the biological process of growing new blood vessels into tissue. For diabetic neuropathy patients, whose microvascular damage has literally starved their nerve fibers of blood supply, this is a powerful mechanism for creating new pathways for circulation and repair.
Shockwave also promotes the release of growth factors that support tissue repair and reduces fibrosis in chronically damaged areas. Patients often notice increased warmth and sensation in treated areas following sessions — hallmarks of improved circulation.
5. Vitamin B12 Injections via Acupoint Injection Therapy (AIT)
For diabetic neuropathy patients — especially those on metformin — B12 deficiency is a critical, frequently missed contributor to nerve damage. Oral B12 supplements are often inadequate because gut absorption is compromised by both diabetes and metformin. We administer B12 by injection directly at acupuncture points, bypassing gut absorption entirely and combining the metabolic benefit of B12 with the neurological stimulation of acupoint therapy.
Methylcobalamin — the neurologically active form of B12 — is the preferred choice for nerve support, superior to the more common cyanocobalamin form found in most over-the-counter supplements. We use methylcobalamin in our AIT protocol.
6. Targeted Nutritional Supplementation
A personalized supplement protocol for diabetic neuropathy typically includes:
– Alpha-Lipoic Acid (ALA): The most researched natural supplement for diabetic neuropathy. ALA is a powerful antioxidant that directly neutralizes the oxidative stress driving nerve damage. Multiple randomized controlled trials support its use for both pain reduction and nerve function improvement in DPN.
– Benfotiamine (Fat-Soluble B1): A highly bioavailable form of thiamine that supports nerve metabolism and has demonstrated benefit in reducing the advanced glycation end-products (AGEs) that damage nerve tissue in diabetes.
– Methylcobalamin (B12): For patients who cannot receive injections as frequently, oral methylcobalamin provides additional support between AIT sessions.
– Acetyl-L-Carnitine: Supports mitochondrial function in nerve cells and has shown nerve regeneration potential in clinical studies of diabetic neuropathy.
– Magnesium Glycinate: Essential for nerve conduction, commonly depleted in diabetes, and often helpful for reducing the muscle cramps and restless legs that accompany DPN.
– Omega-3 Fatty Acids: Reduce systemic inflammation and support nerve cell membrane integrity.
A Word on Diabetic Foot Care
Peripheral neuropathy in the feet creates a dangerous situation: you may not feel injuries when they occur. A small blister, cut, or pressure sore can go unnoticed and progress to a serious wound or infection. For people with diabetes, this is the primary pathway to foot ulcers and, in severe cases, amputation.
Check your feet every single day — including the soles and between the toes. Use a mirror if you cannot see the bottom of your feet easily.
Wear well-fitted, protective footwear at all times — even indoors. Never walk barefoot if you have diabetic neuropathy.
Report any new wounds, redness, swelling, or skin changes to your healthcare provider promptly. Do not wait to see if they heal on their own.
Our office works alongside your primary care physician and endocrinologist as part of your broader diabetes management team. We do not replace your medical care — we expand what is possible within it.
Who We See for Diabetic Neuropathy in Palm Coast
Our diabetic neuropathy patients include:
– Adults newly diagnosed with type 2 diabetes who want to prevent neuropathy from developing
– Patients already experiencing symptoms who have been told to “manage it” with medication alone
– Medicare-eligible seniors with long-standing diabetes and progressive neuropathy
– Veterans with diabetes and service-connected neuropathy (we are a VA Community Care provider)
– Patients on metformin concerned about B12 depletion and nerve health
– Those seeking non-opioid, drug-free options for neuropathic pain management
Part of Our Neuropathy Care Series
This blog is a cluster article within our broader neuropathy education series. Explore related posts:
– Idiopathic Neuropathy: What It Is and How We Treat It — Pillar Blog
– Neuropathy in Veterans: VA Community Care Options in Palm Coast — Published
– Chemotherapy-Induced Peripheral Neuropathy (CIPN) — coming soon
– Small Fiber Neuropathy: A Diagnosis Often Missed — coming soon
– Spinal Decompression and Neuropathy: The Connection You Need to Know — coming soon
Take the First Step Toward Healthier Nerves
If you are living with diabetic neuropathy — or want to be proactive before symptoms worsen — we invite you to schedule a comprehensive neuropathy evaluation at our Palm Coast office.
We accept Medicare and will work with your insurance to identify covered services. Our team will review your diabetes history, current medications, and neuropathy symptoms to build a personalized care plan that addresses your specific situation.
You do not have to accept that burning and numbness are just part of having diabetes. Call us today.
Sources and Additional Resources
– American Diabetes Association — Neuropathy (Nerve Damage): https://www.diabetes.org/diabetes/complications/neuropathy
– National Institute of Diabetes and Digestive and Kidney Diseases — Diabetic Neuropathy: https://www.niddk.nih.gov/health-information/diabetes/overview/preventing-problems/nerve-damage-diabetic-neuropathies
– Foundation for Peripheral Neuropathy — Diabetic Neuropathy Overview: https://www.foundationforpn.org/types-of-peripheral-neuropathy/systemic-diseases/diabetes/
– PubMed — Alpha-Lipoic Acid for Diabetic Neuropathy: Systematic Review: https://pubmed.ncbi.nlm.nih.gov
– PubMed — Acupuncture for Diabetic Peripheral Neuropathy: Meta-Analysis: https://pubmed.ncbi.nlm.nih.gov
– PubMed — Metformin and Vitamin B12 Deficiency: https://pubmed.ncbi.nlm.nih.gov
– American Academy of Neurology — Diabetic Neuropathy Guidelines: https://www.aan.com